The Benefits of Pelvic Floor Therapy
for Men After Prostate Surgery: Regaining Control, Strength, and Confidence
Recovering from prostate surgery can bring relief and hope but it can also come with unexpected challenges. Many men are surprised to experience urinary leakage, urgency, pelvic discomfort, or changes in sexual function after surgery. These symptoms are common, but they do not have to become your “new normal.”
Pelvic floor therapy for men after prostate surgery is a highly effective, evidence based way to support healing, restore function, and improve quality of life. At Klein Physical Therapy, we provide personalized, respectful care to help men regain confidence and return to the activities they enjoy.
Why Prostate Surgery Can Affect the Pelvic Floor
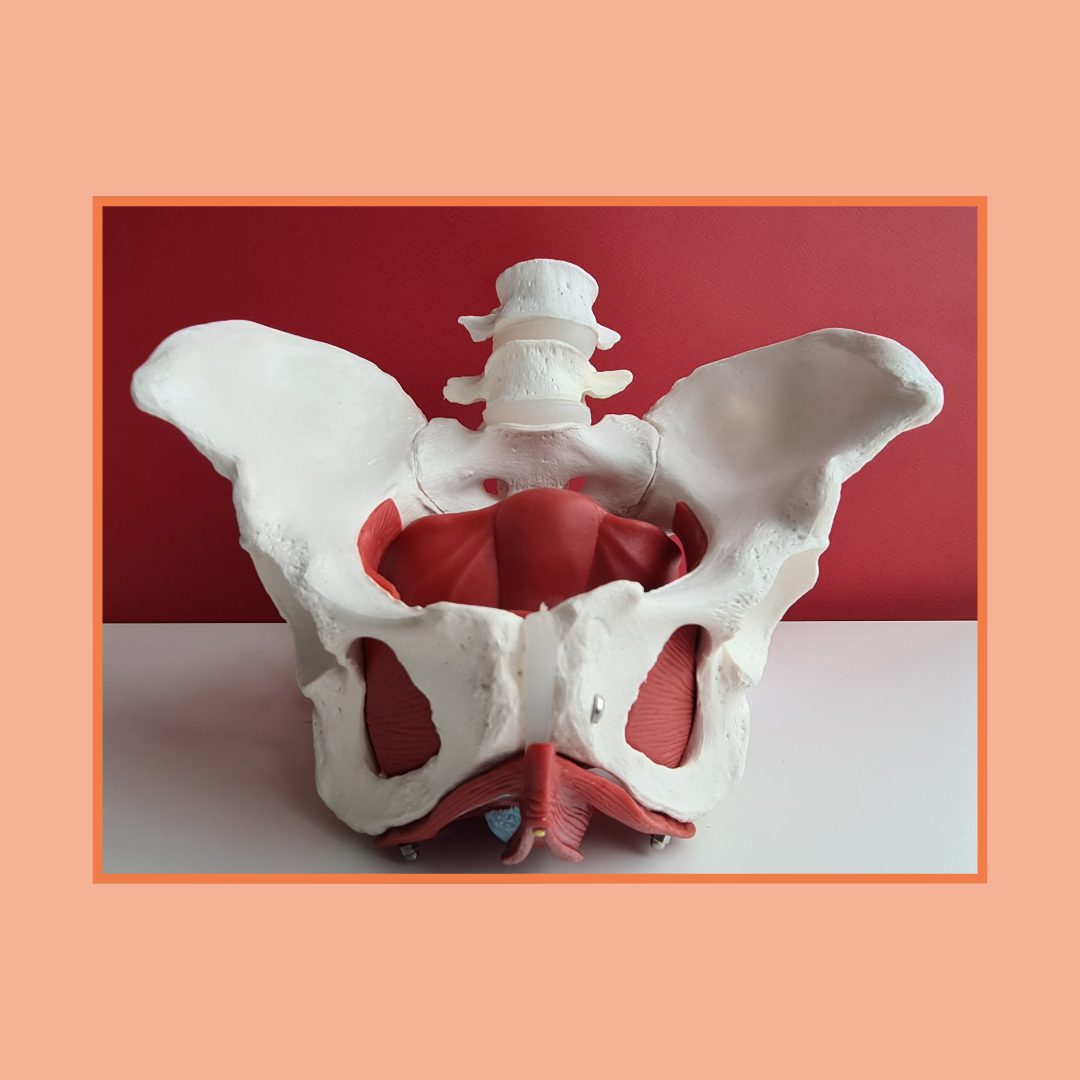
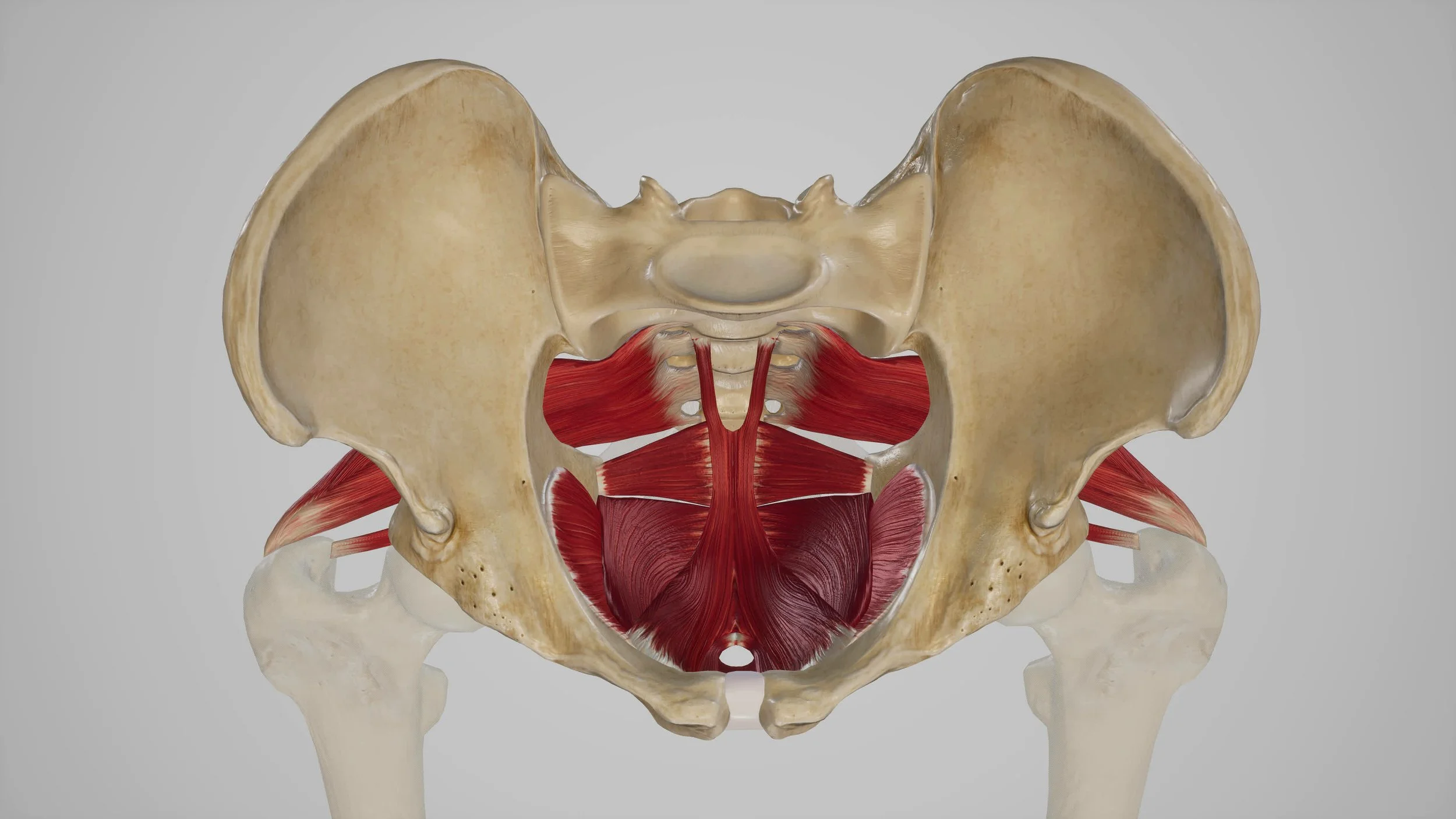
The pelvic floor is a group of muscles, connective tissues, and nerves located at the base of the pelvis. These muscles help support the bladder and bowel, assist with urinary control, contribute to sexual function, and work with your core muscles for stability.
During a prostatectomy or other prostate procedures, the surrounding tissues may be affected by surgery itself, post operative swelling, scar tissue, or changes in nerve signaling. As a result, some men experience difficulty coordinating or strengthening the pelvic floor muscles during recovery.
This is why symptoms such as urinary incontinence after prostate surgery are common and why specialized rehabilitation can make a meaningful difference.
Common Symptoms After Prostate Surgery
Every recovery is different, but many men experience one or more of the following:
Urinary leakage when standing, coughing, sneezing, or exercising
Dribbling after urination
Frequent urges to urinate
Difficulty delaying the urge to urinate
Getting up often at night to urinate
Pelvic tension or discomfort
Weakness with exercise or lifting
Fear of movement or returning to activity
Changes in erectile function or sexual confidence
These issues can impact work, travel, exercise, sleep, and relationships. Fortunately, men’s pelvic floor physical therapy is designed to address these exact concerns.
How Pelvic Floor Therapy Helps After Prostate Surgery
Pelvic floor therapy is a comprehensive approach to retraining the muscles, breathing patterns, posture, and movement strategies that support recovery.
1. Improved Bladder Control
One of the most common reasons men seek pelvic floor therapy after prostatectomy is urinary leakage. Therapy can help you:
Improve pelvic floor strength and endurance
Coordinate muscles at the right time
Reduce stress incontinence (leaking with movement)
Improve control during daily activities
Decrease dependence on pads or protective garments
For many men, targeted therapy helps them feel more comfortable leaving the house, returning to work, or exercising again.
2. Faster, More Efficient Recovery
Healing after surgery takes time, but having a guided plan can reduce frustration and help you progress safely. Rather than guessing what exercises to do, therapy provides individualized strategies based on your symptoms, healing stage, and goals.
This often leads to more efficient recovery and greater confidence throughout the process.
3. Better Core Strength and Stability
The pelvic floor works closely with your diaphragm, abdominal muscles, and back muscles. After surgery, many men feel weak through the core or uncertain about returning to lifting, golfing, yard work, or workouts.
Physical therapy helps rebuild strength in a coordinated way so you can move with more confidence and less strain.
4. Support for Sexual Function
Changes in erectile function can occur after prostate surgery. While recovery may involve multiple factors, pelvic floor rehabilitation can support blood flow, muscle awareness, and coordination that contribute to sexual health.
Many men appreciate having a knowledgeable provider who can guide them through this part of recovery with professionalism and respect.
5. Reduced Pelvic Pain or Tension
Not all pelvic floor muscles need strengthening. Sometimes muscles become tense, guarded, or overactive after surgery. This can contribute to discomfort, urgency, or difficulty relaxing.
Therapy may include relaxation strategies, breathing retraining, mobility work, and gentle movement techniques to reduce tension and improve comfort.
Pelvic Floor Therapy Is More Than Kegels
Many men are told to “just do Kegels,” but without guidance, this can be confusing or even unhelpful if muscles are already tense or if technique is off.
At Klein Physical Therapy, treatment focuses on what your body needs. That may include:
Correct pelvic floor activation
Relaxation training
Breathing mechanics
Pressure management during movement
Scar mobility after surgery
Core strengthening
Bladder habit education
Safe return-to-exercise progressions
Posture and movement retraining
The goal is not simply stronger muscles, it is better function.
What to Expect at Pelvic Floor Physical Therapy
Many men are unsure what happens in therapy and may feel hesitant to schedule an appointment. Our approach is private, professional, and patient centered.
Your evaluation may include:
Discussion of symptoms, surgery history, and goals
Education about normal healing and recovery timelines
Assessment of breathing, posture, core function, and movement patterns
Guidance on bladder habits and fluid strategies
Customized home exercises
A progressive plan to return to work, fitness, and hobbies
We tailor treatment to your comfort level and individual needs every step of the way.
When Should You Start Therapy?
In many cases, pelvic floor therapy can begin before surgery to teach muscle awareness and prepare for recovery. This is often called prehabilitation.
After surgery, therapy can be helpful once your surgeon clears you for rehabilitation. It is also never “too late” to seek help. Even if you had surgery months or years ago and still experience leakage or pelvic symptoms, improvement is often possible.
If you are wondering whether therapy is right for you, it likely makes sense to schedule an evaluation.
Why Men Often Wait Too Long to Get Help
Many men assume leakage or pelvic symptoms are simply something they must live with after surgery. Others feel embarrassed discussing these concerns.
The truth is that these issues are common and treatable. Seeking care is a proactive step toward recovery not something to be ashamed of.
You deserve support that helps you feel strong, capable, and confident again.
Why Choose Klein Physical Therapy?
At Klein Physical Therapy in Denver, Colorado, we take a whole body, individualized approach to healing. We understand that recovery after prostate surgery is not just about one symptom, it is about getting your life back.
Our care is:
Evidence based and personalized
Respectful, private, and compassionate
Focused on real life function and long term outcomes
Designed to help you move forward with confidence
Whether your goal is to stop leaking, return to exercise, improve comfort, or feel like yourself again, we are here to help.
Take the Next Step in Your Recovery
If you are dealing with urinary incontinence after prostate surgery, pelvic discomfort, or changes in function, you do not have to navigate it alone.
Pelvic floor therapy for men after prostate surgery can help you regain control, strength, and confidence.
Contact Klein Physical Therapy today to schedule an evaluation and start your recovery with expert support.